Want to attend the course but can’t make it on this date?
Fill in your details below and we’ll notify you when we next present a course in this area:
South Africa has a rich diversity of spider species, with more than 2000 species. This is directly related to our diverse habitats and landscape in southern Africa. Jumping Spiders are the most specious group followed by Ground Spiders and Crab Spiders. Identification of spiders is tricky, and many new species are described each year (Dippenaar-Schoeman, 2014).
Despite the large diversity of spider species, the Arachnid Unit of the Agricultural Research Council (ARC) reported that only around 50 species of spiders were commonly found inside houses and around human settlements. The majority of these spiders are small species and are harmless to humans. Most spiders avoid humans and rarely come into contact with people. The defensive strategy for many species of spiders is to flee or curl up and drop to the floor. The venom of most common spiders has little or no effect on humans.
There are a number of factors that influence the effect of spider venom on humans. The first factor is that the spider must be large enough to have fair-sized and sharp fangs to penetrate human skin and a reasonable venom yield to cause any toxic effects. Each bite may also be unique due to the volume of venom injected. A venomous spider might give a light defensive bite as a warning and inject little venom with little or no symptoms. The same spider might give a full bite when it is being squashed or hurt. Such a bite may result in severe symptoms. We see this same scenario in snakebites and each bite is completely unique and may not have the same or as severe a reaction as another bite. Bites to different parts of the body may react differently and bites to the head are usually of more concern than to extremities. The age and health of the patient may also influence the bite and children and the elderly are more at risk of severe reactions (du Plessis, 2019).

Severe reactions, in the form of open wounds that may become septic, are sometimes seen from the bites of two groups of spiders in South Africa: The Violin Spiders (Loxosceles species) and Sac Spiders (Cheiracanthium species) (Dippenaar-Schoeman and Jocqué, 1997). Spiders often get blamed for wounds and even doctors are quick to diagnose septic wounds as spider bites. There are no symptoms that are unique to cytotoxic spider bites and bacterial infections cannot be told apart from spider bites. In Africa there are no blood tests or other tests that doctors can run, which can confirm the presence of spider toxins in a patient. Dr Müller of the Tygerberg Poison Centre suggests that bacterial infections are generally the cause of wounds and may occur as a result of scratching the skin with dirty fingers, ingrown hairs, tick bites, mosquito bites and other insect and arthropod bites (Müller et al. 2012). Multiple wounds on a person or multiple people in the same house getting “spider bites” that form wounds are more likely a sign of bacterial infections, as spiders do not bite multiple times or multiple people (du Plessis, 2019). The general rule is that if the spider was not observed biting or found squashed or hurt nearby, it probably was not a spider bite.
The new protocols to vet any spider bite require three steps:
1) The spider must be seen biting or found in the vicinity of the bite at the time of the bite.
2) There must be some evidence of a bite (pain, swelling, redness or itchiness).
3) The spider must be collected or photographed, and identification confirmed by an expert (Herzig et al. 2019)
We often hear of people having deep gaping wounds that are blamed on Sac Spiders. There have even been magazine articles claiming people have had amputations or even died from Sac Spider bites. These magazine stories are untrue. Dr Müller states: “Necrotic arachnidism (a wound from spider bite) is an over-diagnosed clinical entity and is often a convenient diagnosis for unexplained local tissue injury/dermal necrosis.” (Müller et al. 2017).

Sac Spiders are largely nocturnal, and the majority of confirmed bites were reported at night in beds or during the day when victims were attempting to catch and move the spiders (Newlands et al. 1980, Newlands and Atkinson, 1988, Emtsov et al. 2012, Nentwig et al. 2013). African/House Sac Spiders are well documented in houses, especially in the Free State, KwaZulu Natal, Mpumalanga and Gauteng (less common in houses in the Cape provinces) (Müller et al. 2017). In surveys performed by the Arachnid Unit of the Agricultural Research Council, it was found that Sac Spiders accounted for 52% of all 1000 spiders reported from houses in their study. These light brown to yellow spiders are about the size of a R5 coin and have characteristic dark mouth parts. They are often found in houses where they are wandering spiders, not building a web, but may produce a silk sac against a curtain or other suitable surface and may hide under the sac during the day. Historically, bites have been reported as being painful and often resulting in a necrotic wound. They are one of five medically important spiders in South Africa (Dippenaar-Schoeman, 2014)
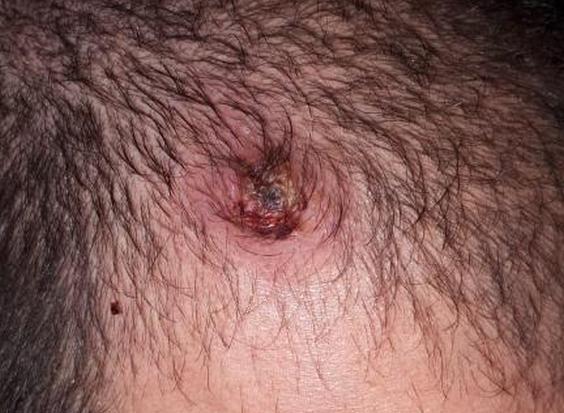
A few recent publications on confirmed Sac Spider bites from Europe, America and Australia have led people to claim Sac Spiders in South Africa are harmless and have since been “declassified” as medically important. This is largely done on social media.
The papers refer to four species of Sac Spiders. European Yellow Sac Spider (Cheiracanthium mildei) and the Eurasian Yellow Sac Spider (Cheiracanthium punctorium) are the most common species in bite reports and investigations. American yellow sac spider (Cheiracanthium inclusum) and the Japanese Yellow Sac Spider (Cheiracanthium japonicum) are also featured in some cases. The papers reported to claim that Sac Spiders are harmless did not include African species and left out important evidence to show the results of venom studies on this group of spiders.
These papers almost all show a painful bite (compared to a wasp or bee sting), erythema (redness), pruritus (itching) and edema (swelling). In about 20% of bites, additional symptoms such as nausea, headaches, vertigo, and general weakness were recorded as well as paralysis of the arm in a paper by Muster (2008). Most studies showed there was no necrosis from the bite and most symptoms disappeared within 45 minutes but could last up to 48 hours (Vetter et al. 2006) or even days (Emtsov et al. 2012 and McKeown 2014). In a few cases (Maretic, 1962, Vetter et al. 2006 and Vetter and Isbister, 2008), small areas of necrosis were observed.
Necrosis, or at least disintegration of the cell (lysis), was reported by Foradori et al. (2005) when they tested the venom of the European Yellow Sac Spider (Cheiracanthum mildei) on sheep blood in lab tests. They tested the venoms of 45 spider species and only the Recluse Spider and Sac Spider showed the ability to break down the membrane of the cells. They did another test by injecting the venom of Sac Spiders into lab rabbits, but the rabbits only showed signs of necrosis after they had injected four times the amount of venom found in a single Sac Spider. However, they had previously frozen the venom which may have denatured the proteins in the spider venom and could alter results. The same test performed by Newlands and Atkinson (1988) where they allowed a live African/House Sac Spiders (Cheiracanthium furculatum) to bite lab rabbits produced necrosis of the tissue that would take up to ten days to heal. Croucamp and Veale (1999) performed the same test with African/House Sac Spider (Cheiracanthium furculatum) venom, and also observed haemolysis (breaking down of blood cells) activity. Spielman and Levi (1970) tested on Guinea pigs and Hamsters with the European Yellow Sac Spider (Cheiracanthium meldei) and showed lesions of the skin, but no necrosis.
Bites by the Eurasian Yellow Sac Spider (Cheiracanthium punctorium) in Russia (Emtsov et al. 2012) didn’t produce necrosis, but showed classic pain, redness and swelling as well as an outbreak of hives in two patients. They also showed that twelve out of nineteen patients had high white blood cell counts, a symptom often seen when the body is fighting a bacteria, virus or venom.
The venom of the European Yellow Sac Spider (Cheiracanthium mildei) was tested by Foradori et al. (2005) and was shown to contain Phospholipase A₂, an enzyme that degrades phospholipids in the skin membrane. Vassilevski et al. (2010) looked at the venom of the Eurasian Yellow Sac Spider (Cheiracanthium punctorium) and found a novel spider toxin they termed CpTx 1. This toxin possesses potent insecticide, cytotoxic and a membrane-damaging activity and tests on insects and frog tissue damaged the cells rapidly. Work by Bosselaers (2013) showed that the molecular mass of the polypeptides found in the venom of the African/House Sac Spider (Cheiracanthium furculatum) was in the range of 14KDA – 200KDA, similar to that of the Eurasian Yellow Sac Spider (Cheiracanthium punctorium). Foradori et al. (2005) also showed that female European Yellow Sac Spider (Cheiracanthium mildei) were almost double as venomous as males producing blood cell disintegration in 65.4% of tests compared to only 38.9% of tests on males. It is well reported that many Sac Spider species are quite defensive/aggressive and females guarding eggs are known to defend the nest against attackers. This was well documented in Papini (2012) where a father and son were bitten by the same female Eurasian Yellow Sac Spider (Cheiracanthium punctorium) guarding an egg sac under a garden chair.

A paper by Dunbar et al. (2019) discussed the formation of necrosis following a bite or sting from an arthropod. There are three ways necrosis is likely to form after a bite and these actions may overlap in many cases.
The first way is that the venom attacks the cell, causing the cell to rupture and die resulting in necrosis. This results in many cytotoxic envenomations.
The second way is necrosis may form after a bite is due to a bacterial infection. Many arthropod bites and stings are often itchy and cause the victim to scratch at the bite site. The scratching may introduce bacteria from the hands/nails of the victim to the wound. Bacteria such as the MRSA Staphylococci is not uncommon in households. Work by Gnädinger et al. (2013) showed that insects and spiders could not spread MRSA even if they had been previously exposed to the bacteria, so it must be introduced to the bite site by the victim her/himself.
The third way necrosis may form is a process termed necroptosis. Necroptosis is a programmed form of necrosis or inflammatory cell death where the body’s immune system causes the cells to die – a term known as apoptosis. Generally, apoptosis is seen when a cell is mutated or dysfunctional and your body will kill off billions of dysfunctional cells a day. These cells, if not destroyed, are what may form cancer in the body. In some spider and insect bites (even if the venom is not particularly toxic) the body may overreact and cause necroptosis resulting in the formation of an area of necrosis around the bite site. The venom itself does not cause the necrosis, but rather causes the body to react. This may explain how the bites of some species that are not particularly toxic may cause severe reactions and even necrosis in some people.
Unfortunately, spiders are often blamed for any festering wound where the cause of the wound is not known. Presumed spider bites that become necrotic appear to be largely bacterial infections and should be treated by a medical professional, usually with wound care management and often a course of antibiotics. If the spider was not observed biting the patient, found at the scene of the bite at the time of the bite and confidently identified by a spider expert, it is unlikely it was a spider bite. Doctors being presented with a claimed spider bite should look at other important causes of dermal necrotic ulcers such as infections (bacterial, fungi, viruses or parasites), tumours, or complications within the blood (Müller et al. 2017). However, all the data presented by various authors across a number of studies suggest that the Yellow Sac Spider and African/House Sac Spider is a venomous species. Bites are generally mild, with pain, swelling, redness and itchiness expected. Occasionally bites may be more severe, and necrosis is a symptom seen in some bites. Due to this, Sac Spiders in South Africa are still considered medically important and these spiders should be treated with respect and caution.
References
CONTACT US:
Product enquiries:
Caylen Steenkamp
+27 60 957 2713
info@asiorg.co.za
Public Courses and Corporate training:
Michelle Pretorius
+27 64 704 7229
courses@asiorg.co.za
 ASI Collapsible Snake Hook - 1.2 m
R650.00
ASI Collapsible Snake Hook - 1.2 m
R650.00
 ASI Book Combo 2
ASI Book Combo 2
 Rangers Book Combo 1
Rangers Book Combo 1
Want to attend the course but can’t make it on this date?
Fill in your details below and we’ll notify you when we next present a course in this area:
Want to attend the course but can’t make it on this date?
Fill in your details below and we’ll notify you when we next present a course in this area:
Want to attend the course but can’t make it on this date?
Fill in your details below and we’ll notify you when we next present a course in this area:
Want to attend the course but can’t make it on this date?
Fill in your details below and we’ll notify you when we next present a course in this area:
Want to attend the course but can’t make it on this date?
Fill in your details below and we’ll notify you when we next present a course in this area:
Want to attend the course but can’t make it on this date?
Fill in your details below and we’ll notify you when we next present a course in this area:
Want to attend the course but can’t make it on this date?
Fill in your details below and we’ll notify you when we next present a course in this area:
Want to attend the course but can’t make it on this date?
Fill in your details below and we’ll notify you when we next present a course in this area:
Want to attend the course but can’t make it on this date?
Fill in your details below and we’ll notify you when we next present a course in this area:
Sign up to have our free monthly newsletter delivered to your inbox:
Before you download this resource, please enter your details:
Before you download this resource, would you like to join our email newsletter list?